We love time in range (TIR) because it makes management easier, but did you know that increasing your time in range can also reduce risk of complications and improve quality of life?
Time in range shows the whole picture of our blood sugar management, which can help us make strategic adjustments to avoid cycling between stubborn highs and stubborn lows like a yo-yo.
Here are a few tips to think about when trying to increase your time in range:
1. Make your CGM work for you—a quick change in settings or alarms make it easier to stay in range
2. When you know more, you can do more—use your data to focus on one time of day that is trickiest for you
3. Be a pattern detective—think about factors in your life and diabetes management that coincide with that time of day
4. One thing at a time—go easy on yourself and focus on changing one thing during one time of the day (diabetes is tricky enough!)
5. A win is a win—celebrate every bit of success. Even tiny changes can make a big difference in how you feel now and down the road.
6. You’re not alone—we’re not pretending this is simple. Asking your healthcare team for help or finding a supportive community of other people with diabetes can make this all less complicated.
Let’s dive into each of these a bit more:
Make your CGM work for you
Try this quick and easy change to make your CGM support your goals. If you’re working with a target range of 70–180 mg/dL, set your CGM’s high alarm lower (maybe around 160) and your low alarm higher (around 80). This gives you a chance to notice you’re headed out of range and shift the direction of your blood sugar trend while you’re still in range.
Keep in mind, this might mean you start getting more alarms. If you’re getting so annoyed with the alarms that you’re tuning them out, take a break and consider trying this strategy again later.
When you know more, you can do more
Identify what times of day you’re often out of range. Pick just one hour within those times to pay more attention to—because while diabetes is a full-time job, we need to save time and energy for other things, too!
So, how do you identify a time frame to focus on? Most CGMs have an accompanying app that helps break down your blood sugar patterns. Some of these apps do the hard work for you, notifying you of trends and the specific times they occur.
Your app also shows your AGP report, which can answer three helpful questions: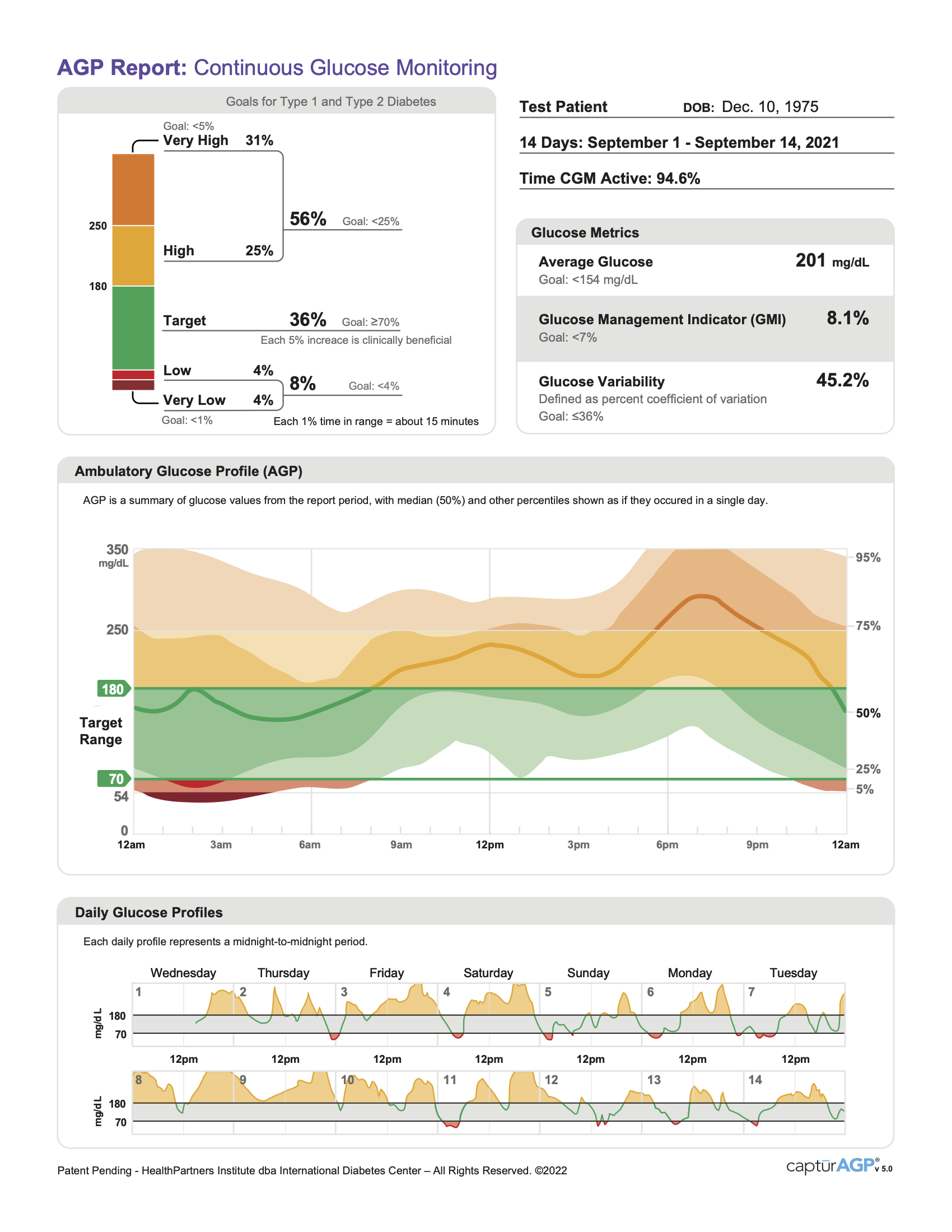
- What time in range goals am I meeting? Identify one goal to focus on – If your time above range goal is just slightly above target, but your time below range goal is much higher than your target, focus there first!
- What time of day am I usually out of range? The graph in the middle of your AGP report can help you easily spot parts of your day when you tend to be above/below your target.
- How are things different day-to-day? At the bottom of the report, you can compare your blood sugar trends from the last 14 days individually. What days are you in range the most? Are weekdays different from weekends?
The data can sometimes be a lot to digest—Consider starting by regularly checking the datapoint that makes the most sense to you, and then check out our resources to keep learning as you get more comfortable.
If your CGM sends you a weekly email report, checking this can be an easy way to build the habit of keeping an eye on your trends and looking for focus areas. As you get more comfortable, play around with the various reports in your app that can help break down patterns by the hour, compare weeks, and more—and focus on the ones you find most helpful.
Research shows that opening your weekly summary emails and learning to interpret your AGP report helps increase time in range, and can make you more confident in your management—so start here!
Be a pattern detective
Once you’ve identified a time to focus on, consider what life looked like when you experienced that pattern. Things to consider include:
-
- Medication: Does your focus area coincide with times you forgot your medication, or were embarrassed to take it in front of others? If you take mealtime insulin, consider the timing of the dose and how accurate your carb estimation might have been.
- Food: There are many complicated factors at play around meals—have grace with yourself! Consider the quantity of carbohydrates, and remember that the type of carb, plus any accompanying protein, fat, or fiber can affect how quickly those carbohydrates are converted to glucose in your bloodstream.
- Exercise: Were you active that day? Some forms of exercise can spike blood sugar mid-activity, while others reduce blood sugar long after you’ve completed your workout—consider whether your focus period is before or after your gym time, and if it looks different on days you did different types of exercise.
- Non-diabetes medications, alcohol, drugs, or caffeine can all affect blood sugar, sometimes in unpredictable ways. Were any of these in the mix during your focus period?
- Hormones: If you menstruate, what phase of your cycle are you in? Notice whether your focus period looks different on a week when you’re on your period, than a week when you’re in your follicular phase. If you’re looking at patterns over a larger period of time, consider longer-term hormone shifts related to puberty or menopause, too.
- How are you feeling? If you’ve been running low on sleep, extra stressed at work, or are feeling under the weather, these can all affect your blood sugar (usually causing it to trend higher).
If you’re at a loss for what could be going on, keep in mind there are at least 42 factors that can affect your blood sugar — taking some time to familiarize yourself with these factors can help as you observe your patterns.
If you’re having a hard time remembering what was going on during the spike last Tuesday that contributed to your focus area pattern (you’re not the only one), explore the features in your CGM app that allow you to log food, exercise, and other notes. A few extra seconds to log these things as they happen can really help with deciphering your patterns later on.
One thing at a time!
Just as we encourage you to pick one hour in the day to focus on, experiment with changing one factor at a time. If you change 5 all at once, you won’t be able to know which ones helped or didn’t, and it will likely be difficult to stick with all of them long-term.
Think about small changes you could make based on the factors you observed that coincide with your focus period. Here are a few examples of things we’ve tried:
- Spikes after a mid-afternoon snack→ Pair carbs with fat, fiber, or protein
- Lows as you arrive at work → bolus a little less for breakfast, knowing the walking during your commute will bring things down
- Stubborn highs after breakfast → Pre-bolus earlier, while getting ready for school before eating
- Highs around bedtime → Try taking a walk after dinner to improve how your body utilizes insulin and fuels your cells
Whether you decide to shake up your exercise routine, hydrate more at work, or adjust your medication for different phases of your menstrual cycle, try to be patient and observant as you learn how these small changes can affect your time in range.
A win is a win
As you see small changes increase the time you spend in range, celebrate that success! Even small changes can make a big difference in how you feel in that moment and down the road. Spending just 15 more minutes a day in your target range boosts your time in range by 1%, and experts say every 5% increase in time in range has a noticeable, meaningful impact on your health and quality of life!
You’re not in this alone!
Remember—no day is going to be 100% in range! Be kind to yourself. Diabetes is complicated, and you’re managing it on top of a life full of many other responsibilities. Your healthcare team is there to help you, so don’t hesitate to ask your doctor about adjusting your medication, or your diabetes educator for a refresher on carb counting. Plus, the diabetes community is always ready to share support and information.

